Fertilization refers to the fusion of a female egg with a male sperm, the first step in the creation of life.
Sometimes the beginning of the journey for a pregnancy is hard. 15% of couples are diagnosed with subfertility, the inability to conceive after a year of regular unprotected sexual relationships [1]. This is frustrating for many couples, in the words of Mason Wheeler:
“It is like your body is rejecting you, like the world has let you down in the worst possible biological way”
Subfertility is usually associated with emotional pain, stress, depression and anxiety. What’s more in societies where women value is measured by their ability to procreate, subfertility problems can lead to social rejection [1].
The causes of subfertility can be associated in approximately 35% of the cases to female causes and another 35% to male reasons. For example, due to absence of ovulation or low egg quality, abnormal sperm or reduced sperm count. However, in 30% of subfertile couples the causes are still unknown [1] .
For the fertilization to happen, the sperm has to travel from the vagina upwards to the fallopian tubes where they will encounter the female egg. Once fertilization has occurred, the zygote (an embryo of just 1-cell) will start growing exponentially at the same time that it travels to the uterus, where implantation occurs. Implantation is the process by which the embryo is embedded into the endometrium that is the lining of the uterus and where the embryo will develop during the next 9 months to develop a new human being [1].
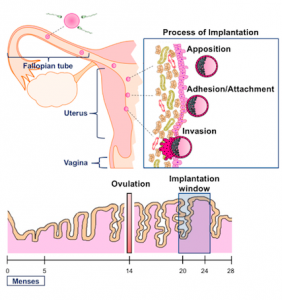
The landmark treatment for subfertility is in vitro fertilization (IVF), and the process of embryo implantation is its main limiting factor. Successful implantation rates are 50-60%, even with very good quality embryos [2]. The process of Implantation can only happen during a specific window of time during the menstrual cycle, which coincides with the time when the endometrium is receptive. Earlier or later attempts of embryo implantation in the cycle will likely result in fail implantation or might lead to later miscarriage or diseases.
In order to prepare the endometrium for implantation, a series of events need to occur. First, the stromal cells in the endometrium suffer functional and morphological changes, a process known as decidualization. As well, the immune system is modulated to prevent the rejection of the embryo. Finally, the communication between the endometrium and the embryo is crucial for a successful pregnancy. To exemplify the changes that occur during this process, let’s imagine a building site. In order to build a building, you need several elements: the bricks, the painting, the builders. In this scenario, the bricks are the building blocks that provide support and structure to the walls, which would be the equivalent to the endometrial stromal cells. The paint interacts with the outside and also protects the underlying bricks; they would be representing the endometrial epithelial cells. The builders are in charge to make sure that the building is properly built and that the walls don’t get damaged, a job equivalent to that of the immune cells. Imagine now that the building is being remodelled to include a new room. In pregnancy, that would be the developing embryo. In this scenario, the building layout has to change. Some brick walls need to be broken down to build the new room and these bricks will then be re-used and walls will be re-painted. This job will be done by the builders very carefully, as they want to adapt the space without destroying the whole building. That is similar to what the endometrium undergoes to reach receptivity. However, if any of these things goes wrong, embryo implantation will fail [3].
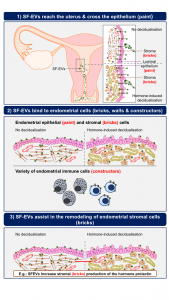
Although this seems very complex, new studies are searching for possible solutions to increase the success rate of IVF. It has been shown that exposure to seminal fluid during IVF treatment can improve implantation rates, suggesting that males might help increase successful implantations. The seminal fluid contains large amounts of vesicles that are secreted by cells, known as extracellular vesicles. They are like bubbles that contain information inside them, the cargo, which is important for cell to cell communication. These vesicles, called Seminal Fluid Extracellular Vesicles (SF-EVs), are important to ensure that the sperm works properly. For example, they prevent the premature maturation of the sperm, which would impede the later egg-sperm fusion from happening [4].
In the pursue to find new ways to improve the implantation of the embryo during IVF, my PhD research focused on these vesicles. I discovered that they can increase the receptivity of the endometrium. Together with other studies, I proposed a model that suggests these vesicles can travel to the uterine cavity thanks to the reproductive tract movements and that the sperm can carry them. There, they interact with the immune cells (builders), the epithelial cells (paint) and the stromal cells (bricks) in the endometrium to prepare it for the implantation of the embryo.
These findings open a door to low-cost and non-invasive interventions that could improve the implantation of the embryo in IVF treatments, and would benefit these women that, after undergoing assisted reproduction, still fail to become pregnant.
By Helena Rodríguez-Caro (@HelenaRodriCaro), post-doctoral researcher at the Department of Physiology, Anatamoy and Genetics at Oxford University.
More information: