I am a pharmacist with a PhD in Medicine and Human Physiology, but I also hold another degree that sometimes might not get as much attention nor recognition as it should: I am a mum (a skeptical one, at the beginning of the maternal journey…). With the authority that these two degrees grant me, I have written this post about breastfeeding where I explain why it is good and how it is successfully done from a physiological point of view.
Breastfeeding is probably the only physiological process that has become a social debate. For those who are not familiar with the term, physiological refers to a normal function, i.e., something that usually occurs in your body.
While breastfeeding has been working for the vast majority of women from the beginning of humanity, formula feeding appeared less than a century ago during WWII to fulfill the milk requirements millions of baby orphans had. Therefore, breastfeeding VS formula feeding is just a recent debate discussed in today’s society.

There is a social debate when it comes down to choose between formula milk feeding and breastfeeding.
When a woman has to decide how she wants to feed her baby, there is usually a lack of accurate information, a reason for this social debate to still be a health issue for the World Health Organization (WHO). For instance, the recommendations about breastfeeding related to health from many international recognized organizations (such as WHO and UNICEF) are usually not known by the mother or by health professionals around her, which creates a huge information gap. And misinformation is ALWAYS a problem.
Physiology of the mammary gland
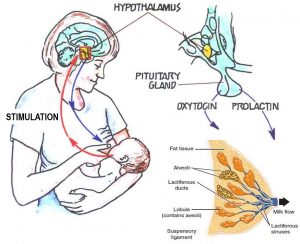
Physiological mechanisms of breastfeeding. Role of baby’s suckling to induce the secretion of prolactin and oxytocin hormones.
Milk is produced by the cells of the mammary gland, stored in alveoli and finally secreted through lactiferous ducts. Milk production depends on the hypothalamic hormone prolactin, whereas milk ejection depends on the hypophyseal hormone oxytocin. Both hormones depend on the effective suckling of the baby. In other words, the central dogma of breastfeeding is that milk production by the mammary gland is adapted to the baby’s demand through effective suckling. To increase milk flow, the baby has to nurse more. These physiological processes work for most women, in the same way that other endocrine glands do. Hypogalactia or agalactia (little or no production of milk) are endocrine pathologies.
A glimpse of anthropology…
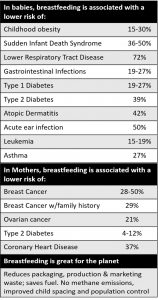
Breastfeeding results in improved infant and maternal health outcomes, such as reduced incidence of several diseases [1, 3]. Furthermore, breastfeeding is also a more environmentally-friendly than the alternative formula feeding.
Let’s now take a look at some anthropological facts. Humans have a significantly bigger brain than any other mammal. This fact, together with bipedalism (i.e., standing up on two feet), causes the pelvis to narrow, thus leading humans to a shorter gestation than desirable. Consequently, significant brain growth, behavioral development, and maturation of systems are all to be completed beyond birth. This scenario is not necessarily deadly, because the composition of human milk helps to reach full growth, development, and maturation of such systems [1, 2]. Some examples are given below:
- Immune system: human milk contains antibodies and defense cells (around 1000 cells/drop!), providing the baby’s immature immune system with the necessary immunity.
- Digestive system: human milk stimulates the growth of good bacteria (physiological microbiota) and oligosaccharides, which prevent gastrointestinal diseases.
- Endocrine system: hormones and growth factors present in human milk help to prevent endocrine diseases such as diabetes or obesity.
- Bones and cartilages: calcium and phosphorus, both mineral components of bones, are much better absorbed from human milk than from formula milk because they are bound to the proteins. Moreover, the triglyceride structure of human milk, different from that of formula milk, promotes calcium absorption and reduces colic episodes in infants.
- Neurological (nervous) system: composition of human milk helps to complete the development of the brain with its superior functions, as well as the senses and the circadian rhythm. This last one is very important for both mums and dads: the sooner the baby can differentiate night from day, the better for the whole family!
All those benefits have one thing in common: the composition of human milk. If compared to formula milk, human milk has more of “the good things”: immune cells, hormones, enzymes, growth factors, healthy microbiota, and antibodies. Besides, the quantity and bioavailability of common components in both kinds of milk are actually much higher in human milk. Considering all these reasons, breastmilk is the gold standard nutrition for the newborn due to its potential to prevent several pathologies during infancy and beyond [3]. There are also many proven benefits for the mum [4] such as less anemia, lower risk of several serious diseases such as cancers (e.g., breast, ovarian, etc.), cardiovascular diseases, post-partum depression, fewer multiple sclerosis episodes, faster weight loss and back to normal size of the uterus after delivery, contraception, etc.
All in all, breastfeeding is definitively a cheaper option and much more convenient for most women. Some of them even refer to it as a much easier and less exhausting process as the baby is normally fed before going to sleep. Finally, according to many mothers’ experiences, breastfeeding is like a magic solution for all sorts of problems: nightmares in the middle of the night that disappear with breastfeeding because children fall asleep almost immediately, secure nutrition and hydration when the baby is sick and they are not eating well (i.e., breast milk will always give calories and nutrients), small brushes that all of a sudden are forgotten when the child begins suckling, etc.
Then, why not feeding human babies with formula milk?
There are some facts about formula milk that you may not know. To start with, commercial formula milk is actually cow milk [5] with additives such as vegetable oils and processed to have less amount of proteins and fat (calves are much bigger than human babies are). This industrial treatment of cow milk reduces protein and fat contents to non-toxic levels, but they are still higher than optimum levels. This can cause renal overload to human babies’ kidneys. Besides, formula milk does not have antibodies or defense cells, hence not providing the baby with any immunity.
The final decision
There are many different reasons why a mum could choose formula feeding over breastfeeding: very little time to adjust to changes of postpartum, non-supportive family or health professionals, embarrassment, lack of confidence, feeling of little or no production, medication, back to work, nipple soreness, overwhelming process… However, most of the times this is mainly due to a LACK OF ACCESS TO ACCURATE INFORMATION. The truth is that almost every pitfall that a mother can encounter usually has an easy solution. It is just a matter of when, where, and who to ask for help. Therefore, in order to make the best decision about how to feed your newborn, mothers should be responsible for seeking information from the beginning of their pregnancy: ASK, READ, SEARCH, UNDERSTAND… AND THEN, ASK AGAIN.
Besides, it is essential to keep health professionals accurately informed about how to promote, initiate, and maintain breastfeeding; even when the mother gets back to work and/or is on medication. Everybody involved in breastfeeding should get rid of prejudices about certain issues such as how long it should last (WHO recommends exclusive breastfeeding for the first 6 months and combined with other complementary food for, at least, 2 years), co-sleeping, the potential embarrassment to breastfeeding in public, etc.
In the end, this is always a personal choice. Nevertheless, this final decision should be made after having considered all the available information about it, especially everything health-related.
* * *
By Maria del Carmen Iglesias de la Cruz, Professor of Physiology at the Department of Physiology at the Faculty of Medicine (Universidad Autónoma de Madrid).
More information:
- Dieterich, C. M., et al. Pediatr Clin North Am. 2013.
- Nigatu, D., et al. PloS one. 2019.
- Eidelman, A.I., Schanler, R.J., et al. Pediatrics. 2012.
- Chowdhury, R., et al. Acta Paediatrica. 2015.
- Martínez, J.A., et al. Pediatr. Rev. 2011.
- Blog about “11 benefits of breastfeeding”.
- Blog about “I know how to end the breastfeeding VS bottle debate”.
- Blog about “Breast bottle feeding”.