I am confident to say that most of you have heard before that true beauty lies in laughter lines and wrinkles. Despite its rather positive message, this sentence is only partially true in our current society mostly obsessed with physical appearance and public opinion, where happiness actually ends with the formation of the first wrinkles. Our obsession with beauty is most likely the main reason why we may be familiar with the hyaluronic acid, the so-called “miracle substance of beauty”. What’s more, you may have already noticed its ubiquitous presence in today’s cosmetic products and food supplements as seen on TV, website and magazine ads, or even at the supermarket or the chemist’s. But, ¿what is hyaluronic acid? ¿do you think its use is limited to anti-ageing science? ¿would you believe me if I told you it is in fact one of the most researched molecules in the search of a cure for cancer? In this post, I will try to introduce you to the science around this polymer, focusing on why it is so valuable in cosmetic applications, and, in particular, why it is now considered a “true miracle” in the fight against cancer.
Hyaluronic acid is a big sugar molecule composed of repetitive units of two smaller sugars: N-acetyl-D-glucosamine and D-glucuronic acid (Figure 1). This polymer is found in nature as one of the main components of the structural and biochemical support meshwork essential for cell growth, cell communication and organ formation: the extracellular matrix.
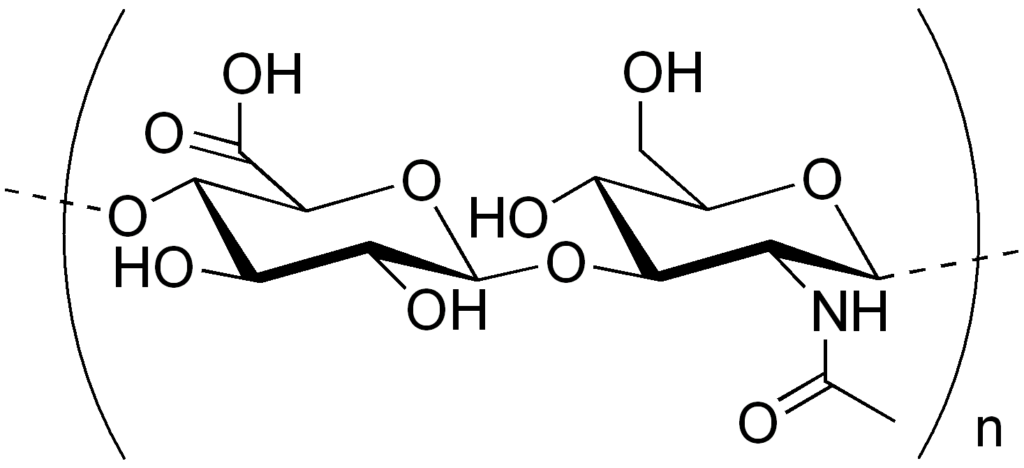
Figure 1. Chemical structure of hyaluronic acid.
The key structural function of hyaluronic acid in this matrix stems from two characteristics: its high hydrophilicity, i.e. its ability to attract and hold water (one molecule of hyaluronic acid can retain 1000 times its weight in water!), and its multiple interactions with other proteins to form more complex structures. In fact, these hyaluronic acid structures are really abundant in the synovial liquid, a fluid which is found filling our joint cavities with a key role as a lubricant and cushion for joint cartilage; and in the skin, where it is critical in maintaining its hydration and adding thickness and volume, thus ensuring its smoothness and tonicity. Approximately half of the hyaluronic acid in the body is found in the skin during our youth; however, both its skin content and our ability to replenish it decrease dramatically with age, which in turn triggers wrinkles formation and skin flaccidity. Therefore, it is not surprising that the exogenous administration of hyaluronic acid, as part of cream formulations or as dermal fillers, has been successfully used to tackle the signs of ageing and to contour various body parts. This is probably the most profitable application of hyaluronic acid, especially after the optimization of its batch production.
Nevertheless, hyaluronic acid is not simply a structural and inert component of the extracellular matrix as the scientific community used to believe up to the seventies, but it actually regulates a myriad of physiological processes in the body through its interaction with cellular receptors. In particular, the interaction of hyaluronic acid with its main cell surface receptor, CD44, modulates cell-cell and cell-substrate adhesion processes, lymphatic degradation of hyaluronic acid, cell growth and migration, and the formation of new blood vessels, among others. The last two are intimately associated with certain pathologies. For instance, both uncontrolled cell division and migration from a primary site to a secondary site are typical processes in cancer (Figure 2).

Figure 2. The process of cancer metastasis in which hyaluronic acid-associated molecules play a key role.
Indeed, a number of scientific studies has highlighted the key role of CD44 and its abnormal expression in most human solid tumours, where this receptor regulates various malignant processes in order to create a receptive environment for cancer cells to migrate to secondary organs. In particular, a high amount of CD44 is now considered as a clinical marker of “cancer stem cells” – a chemo- and radio-resistant cell subpopulation responsible for metastasis and tumour relapse. The possibility of using increased amounts of CD44 to target drugs to such cell subpopulation proves promising to the development of new anti-cancer therapies, based on the conjugation or decoration of drugs and other novel materials, such as nanoparticles, with hyaluronic acid. Thereof, it is expected that treatment would target these drugs preferentially to tumoral cells due to the great amount of CD44 present in those in comparison to healthy cells. While some studies have showed satisfactory results in animal models and clinical trials, even reducing size of several tumour types such as colon or pancreas, others have casted doubts about the ability of certain cancer cells to constantly bind hyaluronic acid. This scenario greatly complicates such therapeutic approach: there is neither two patients with exact same profiles, nor different tumours within the same patient. Although there is an outstanding amount of future work to be done in this field, we can affirm the hyaluronic acid revolution is here to stay, and its use in research is paving the way for a number of strategies to treat cancer and surpass the limitations of conventional therapy.
By Julio Manuel Ríos de la Rosa, PhD student, NorthWest Centre for Advanced Drug Delivery (NoWCADD), School of Health Sciences, University of Manchester. SRUK NorthWest Constituency.
Abbreviations: hyaluronic acid (HA), hyaluronic acid synthase (HAS), hyaluronic acid receptor (HAR), hyaluronidase (HAase).
More info:
NOWNANO DTC PhD program